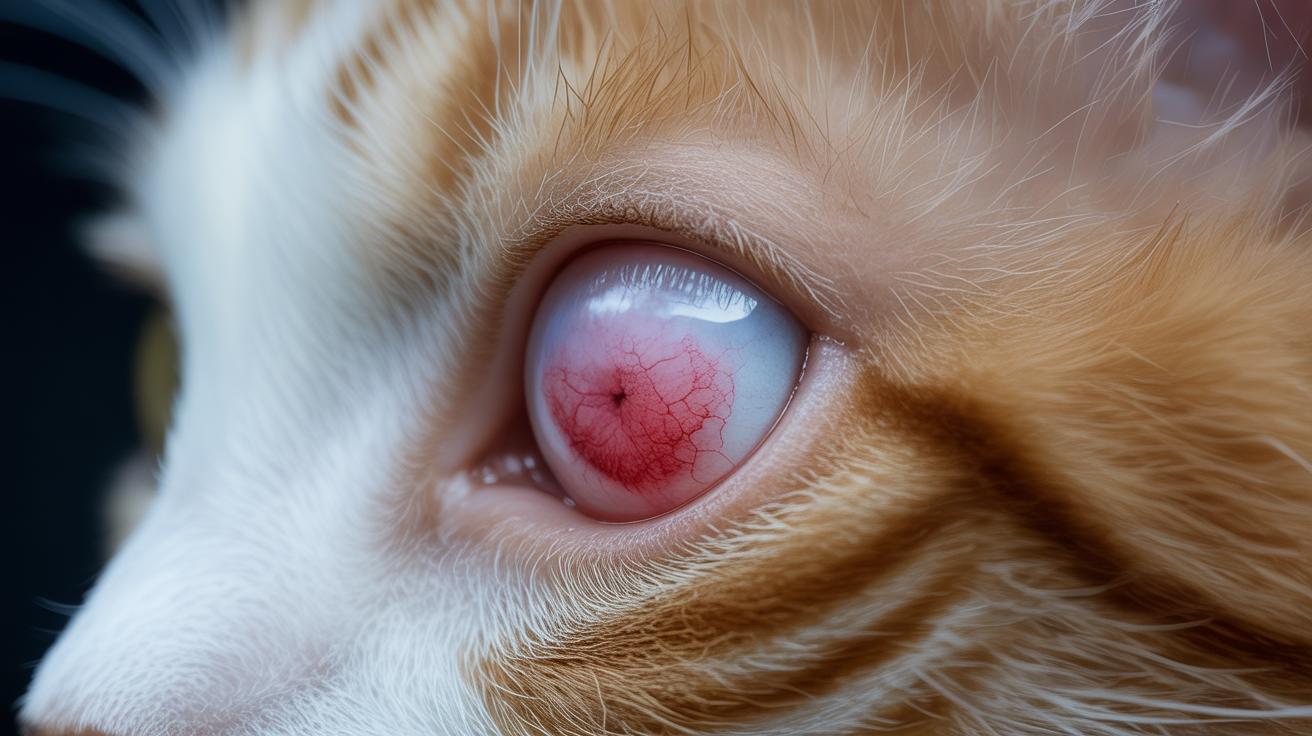
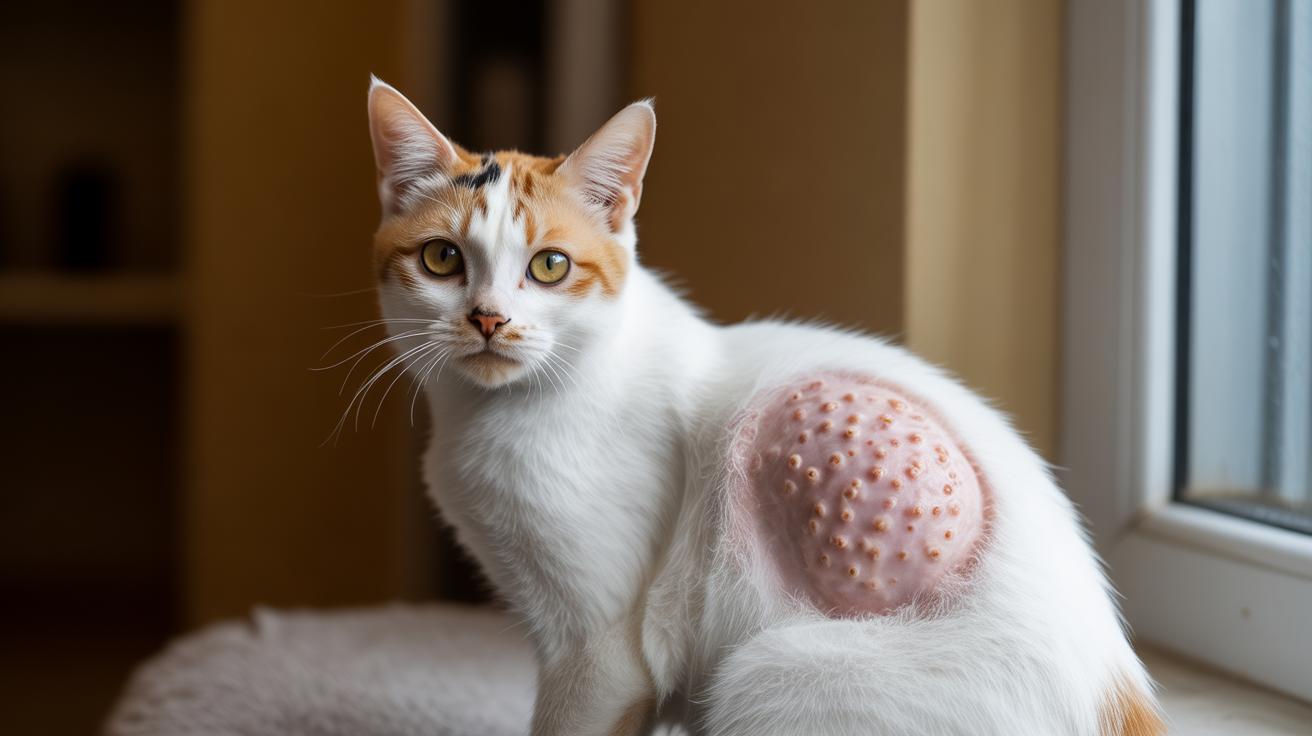
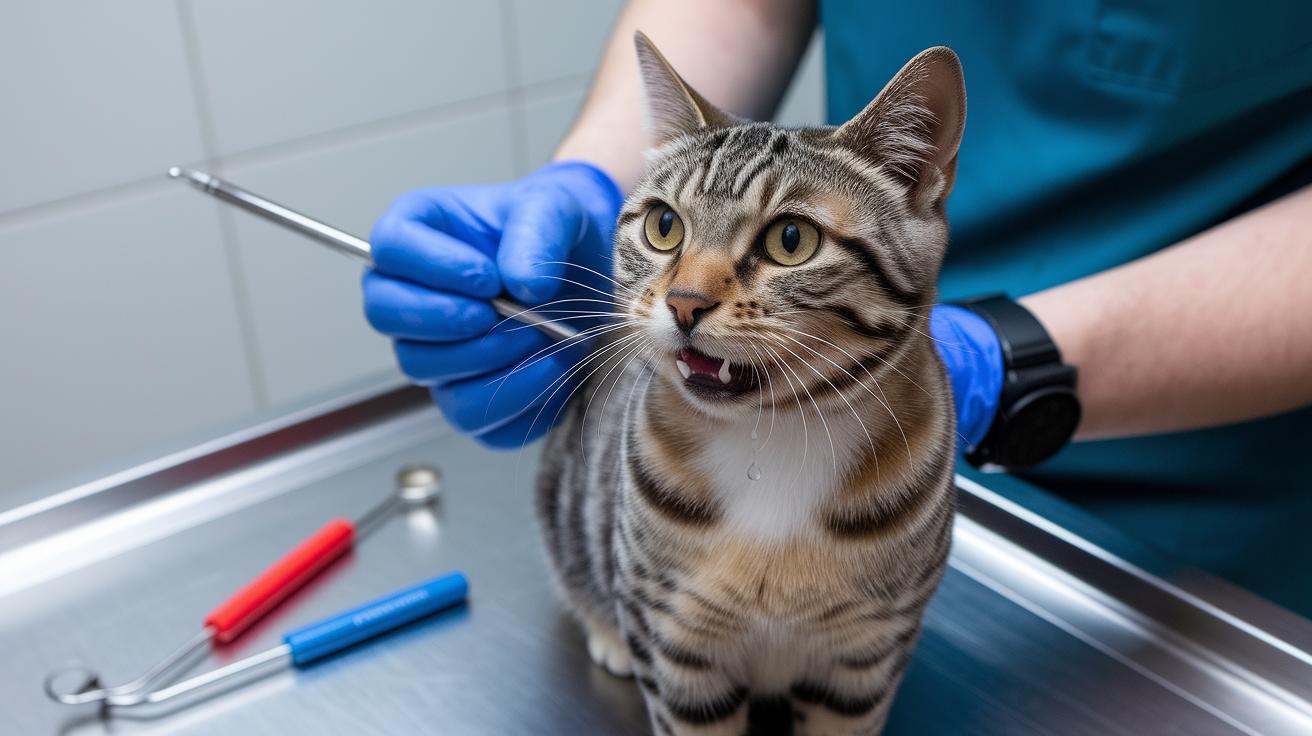
See blood in the litter box? Don’t shrug it off. That pink puddle can mean something as simple as a urinary tract infection (UTI) or as dangerous as a urethral obstruction (a plug or blockage in the tube that carries urine out), so it deserves a quick check.
Common causes include urinary tract infection (UTI) , germs that bug the bladder , bladder stones (hard mineral lumps that irritate or block the bladder), cystitis (bladder inflammation), and clotting disorders (when blood doesn’t clot properly). Tiny crystals (small mineral bits that can form stones) can show up too and start trouble. Each one feels different to your kitty, but they all can make peeing painful or bloody.
Watch for emergency signs like straining in the box, repeated short trips with little or no pee, loud crying while trying to pee, a hard or swollen belly, vomiting, or sudden weakness. If your cat is struggling and producing almost no urine, go to a vet right away , this can become life-threatening in a matter of hours. Ever watched a cat try and fail to pee? Heartbreaking.
Basic tests your vet might run include urinalysis (a urine test that checks for blood, crystals, and bacteria) and sometimes bloodwork to look at kidney function. Quick first-aid at home: stay calm, keep your cat warm, offer fresh water, and try to collect a small urine sample if you can (a clean shallow container or a plastic bag on the litter works in a pinch). Don’t try to squeeze the bladder or give human meds, okay? Pack the cat carrier and see your vet if you notice any worrying signs.
You’ll feel better getting it looked at , and your cat will too. Worth every paw-print.
Rapid answers for blood in your cat's urine: why it happens, how serious it is, and what to do now

If your cat is straining with little or no urine, go to an emergency clinic now.
- Keep your cat safe and stay calm. Close them in a quiet room so they don’t panic.
- Watch to see if they are straining and whether any urine comes out.
- If you can, collect a urine sample or snap a photo of the urine or soiled litter , that can help the vet.
- Don’t give antibiotics or other meds at home, and keep your cat away from possible toxins.
- Call your regular clinic or an emergency clinic and head there right away if you think there might be a blockage.
Watch for these emergency signs:
- Straining with little or no urine.
- Repeated vomiting.
- Collapse or not responding.
- Open-mouth breathing or trouble breathing.
- Extreme sleepiness or not waking up.
- A hard, swollen, or painful belly.
A urethral obstruction (a plug or blockage in the tube that carries urine out) can get dangerous fast. If it’s not treated, your cat can get kidney failure, a life-threatening electrolyte imbalance (too much potassium), or the bladder could rupture within 48 to 72 hours. If you suspect a blockage, getting to an emergency vet quickly is critical.
Do not try to put in a catheter at home , you can hurt the urethra or push the plug in further. Don’t give antibiotics without a vet’s advice; the wrong drug can hide signs or harm the kidneys. Bring a fresh urine sample or clear photos of urine color or soiled litter if you can, plus any recent medicines and a short history of the signs you’ve seen.
For full diagnostic-test descriptions and the official clinic test table, see the "How vets confirm hematuria" section, which outlines urinalysis (checking urine for blood, crystals, infection), culture (growing bacteria to identify infection), bloodwork (checking organ function and electrolytes), and imaging (x-rays or ultrasound) that vets use to find the cause of blood in a cat’s urine.
Ever watched your kitty’s whiskers twitch while they try to go? It’s scary when things go wrong, but quick action really helps.
Causes of Blood in Cat Urine

Seeing blood in your cat’s urine is scary, and it’s one of the top reasons folks call the vet. The common culprits are FLUTD, urinary tract infection, and bladder stones, and each can make your kitty pee outside the box, strain, or produce bloody or discolored urine.
FLUTD, which stands for feline lower urinary tract disease, is basically sterile bladder inflammation (bladder irritation without bacteria). It often hits young to middle-aged cats under stress and causes lots of trips to the litter box, tiny amounts of urine, and sometimes blood. It’s usually not an emergency unless the cat becomes blocked.
A urinary tract infection (UTI) is more common in older cats and in females. With a UTI you’ll often see painful, frequent urination and visible blood. Prompt vet care is a good idea.
Bladder stones and crystalluria (tiny mineral crystals in the urine) can show up at any age, but certain kinds of stones are more common in middle-aged to older neutered males. Stones are hard mineral lumps that can cause pain, repeat infections, or even blockages. Some cases need surgery.
Urethral plugs or obstructions are most common in neutered males and cause straining with little or no urine, plus severe pain. This is an emergency. Get your cat to an emergency clinic right away.
Trauma to the urinary tract after a fall, fight, or accident can cause visible blood and pain at any age, so urgent evaluation is wise. Coagulopathy (a bleeding disorder that makes blood not clot properly) can cause bleeding from multiple places, including the urine, and may be life-threatening.
Bladder tumors (cancer) occur more often in older cats, usually over ten, and often cause persistent blood in the urine and weight loss. Kidney disease or pyelonephritis (a kidney infection) tends to affect older cats and can cause darker or bloody urine plus lethargy or vomiting; these sometimes need quick treatment.
Intact females can have reproductive tract bleeding (uterine or vaginal bleeding) that looks like bloody urine and should be checked by a vet.
Visible blood can be pink, brown, bright red, or come with clots, and sometimes the blood is microscopic and only a vet will find it. Other signs that vary by cause include changes in how much your cat pees, odd urine smell, vocalizing while peeing, or extra licking around the genitals. Ever watched your cat make everything dramatic around the litter box? Yeah, that’s the one to watch.
Match your cat’s signs to the short list below to help the vet triage quickly:
- FLUTD/FIC (sterile bladder inflammation): Often young to middle-aged cats of any sex, stress-related frequent urination, blood, and litter-box avoidance; usually not an emergency unless blocked.
- Urinary tract infection (UTI): More common in older or female cats, painful and frequent peeing with visible blood; prompt vet care is typical.
- Bladder stones/crystals: Seen in middle-aged to older cats and often neutered males; signs include straining and blood and may need urgent care or surgery.
- Urethral plugs/obstruction: Most common in neutered males, causes straining with little or no urine and severe pain. This is an emergency.
- Trauma to urinary tract: Any age after a fall or fight, shows blood and pain; urgent evaluation advised.
- Coagulopathy and bleeding: Can affect cats of any age, causes bleeding from multiple sites including urine and may be life-threatening (bleeding disorder).
- Bladder tumor: Tends to occur in older cats with persistent blood and weight loss; needs a thorough workup.
- Kidney disease/pyelonephritis (kidney infection): Usually older cats, may cause darker or bloody urine plus lethargy or vomiting and can need fast treatment.
- Reproductive tract bleeding: Intact females can have uterine or vaginal bleeding that may look like bloody urine and requires veterinary assessment.
For which diagnostic tests are typical for each cause, refer to the "How vets confirm hematuria" section for full descriptions and the diagnostic table.
How vets confirm hematuria in cats: tests you can expect at the clinic

When a vet looks into blood in your cat's urine, they follow a clear, step-by-step plan. First they take a focused history and do a physical exam, then they test the urine, check bloodwork, and image the urinary tract if needed. Think of it like building a puzzle, each test adds a piece until the picture makes sense. Ever watched your kitty stare at a puddle and you wonder why? Yeah, this is the clinic version of that curiosity.
- Take a detailed history and do a physical exam.
- Run a urinalysis (urine test) and examine urine sediment (microscope check of particles).
- Send a urine culture and sensitivity (grow any bacteria and find the best antibiotic) when infection is suspected or before a long antibiotic course.
- Perform a CBC (complete blood count) and blood chemistry panel (blood chemistry, including electrolytes and creatinine – kidney marker).
- Use abdominal ultrasound (sound-wave imaging that shows soft tissues) to look for stones that don’t show on x-ray, masses, and subtle kidney changes.
- Take radiographs (x-rays) when radiopaque stones (stones that show up on x-ray) are likely or to screen for other changes.
Urinalysis uses a dipstick (a quick chemical strip) plus a microscopic sediment exam (looking for red blood cells, crystals, bacteria, and cells). Dipsticks are fast but can give false positives from foods, cleaning agents, or contamination, so the sediment exam tells the real story and can catch microscopic hematuria you wouldn’t see with the naked eye. Urine culture and sensitivity takes about 48 to 72 hours, and it helps pick the right antibiotic for a clear infection or for recurrent problems.
Cystocentesis (taking urine with a needle straight from the bladder) gives the cleanest sample for culture and lowers contamination risk, but a vet must do it because there is a small risk of bleeding or poking something if the bladder is tiny or scarred. Catheterized samples can be useful sometimes, but they may introduce bacteria or need sedation in male cats, so your vet will choose the method that fits your cat’s situation.
Bloodwork checks for infection, dehydration, how the kidneys are doing, and dangerous electrolyte problems like high potassium (a salt your body uses for heart and nerve function). Imaging choices: radiographs (x-rays) pick up radiopaque stones; ultrasound finds nonradiopaque stones (stones that don’t show on x-ray), bladder masses, and subtle kidney changes. If a mass shows up or the cause stays unclear, the vet might suggest cystoscopy (a camera into the bladder) or a biopsy (tissue sample).
Sample collection tips: a voided or free-catch sample is the easiest, but it can be contaminated. Use a clean container, keep the sample chilled, and try to get it to the clinic within two hours. Bring a list of recent medications, a photo of discolored urine if you have one, and a short timeline of signs. Rechecks are common. For example, we usually recheck urinalysis 7 to 14 days after finishing treatment for a simple UTI, and follow-up is longer for kidney infections or stones.
| Test | Purpose | What it reveals |
|---|---|---|
| Urinalysis | Quick screen for blood, protein, glucose, and pH | Shows visible versus microscopic hematuria, urine concentration, and clues to infection or crystals |
| Urine culture | Identify bacterial infection and antibiotic sensitivity | Grows bacteria and guides targeted antibiotic choice (results about 48 to 72 hours) |
| Urine sediment | Microscopic exam of cells, crystals, and organisms | Confirms red blood cells, white blood cells, bacteria, and crystal type |
| CBC / Chemistry (including electrolytes) | Assess overall illness and organ function | Finds anemia, signs of infection, kidney values, and dangerous electrolyte imbalances |
| Abdominal ultrasound | Detailed look at bladder, kidneys, ureters, and masses | Finds stones that don’t show on x-ray, tumors, inflammation, and subtle kidney structure changes |
| Radiographs | Screen for stones that show on x-ray | Shows dense stones like some struvite or calcium oxalate stones when they are dense enough to appear |
Urinary tract infections and kidney infections: presentation, treatment, and timelines

A urinary tract infection in cats can involve the bladder (where urine is stored), the urethra (the tube urine leaves through), the ureters (tiny tubes that carry urine from the kidneys), or the kidneys themselves. You might notice blood in the litter box, more trips to the box, straining, or crying while your cat pees. Sometimes the signs are subtle, like lingering at the box or licking down there. Older cats and females tend to get bacterial UTIs more often, but any cat can be affected. Ever watched your kitty freeze and stare while trying to pee? Yeah, not fun.
When the infection moves up into the kidneys it’s called pyelonephritis (kidney infection). That’s deeper and tougher. Cats with pyelonephritis often seem sick overall , fever, not eating, and vomiting, on top of dark or bloody urine.
Vets confirm a UTI with a urinalysis (a dipstick test plus looking at the urine under a microscope). They’ll usually send a urine culture and sensitivity (growing the bacteria to choose the right antibiotic) when infection is likely or before starting a long antibiotic course. For full test descriptions and timing, see the "How vets confirm hematuria" section. Hydration helps the whole process , offering canned food or giving supervised subcutaneous fluids (fluids given under the skin) can ease the kidneys while medications work.
- collect urine for urinalysis and culture
- give a targeted antibiotic chosen from the culture results (antibiotic selection for cats)
- provide pain control if your cat seems uncomfortable
- recheck urinalysis and culture at the end of treatment
- keep fluids up and watch litter-box output
Uncomplicated lower UTIs often start to feel better in days and are usually clearer within a week with proper treatment. Kidney infections usually need a longer antibiotic course, commonly 4-6 weeks. Follow-up testing (repeat urinalysis and culture) helps confirm the infection is truly gone. Isn’t it nice when a treatment actually works? For a practical owner resource on prognosis and recurrence, see Do cat UTIs go away.
Bladder stones, crystals, and urethral obstruction: types, risks, and emergency potential
Stones are hard mineral lumps that form in the kidneys, ureters (tiny tubes that carry urine from the kidneys), or bladder. Crystals (crystalluria – tiny mineral bits seen in urine) can show up on a test even when no stone is present, especially if the urine is concentrated. Vets confirm what’s going on with a urinalysis (lab check of urine), radiographs (x-rays), and ultrasound (sound-wave imaging) – see the "How vets confirm hematuria" section for the full clinic test details.
Struvite and calcium oxalate are the two most common types, and they act differently. Struvite stones (made of magnesium ammonium phosphate – a mineral salt) often respond to a prescription diet that dissolves them. You’ll usually see these in younger to middle-aged cats. Calcium oxalate stones (hard mineral lumps) don’t dissolve and most of the time need surgery to remove. These are more common in middle-aged to older neutered males.
Other types you might hear about:
- struvite (younger to middle-aged cats; often dissolves with a prescription diet)
- calcium oxalate (middle-aged to older neutered males; usually needs surgical removal)
- urate (rare; linked to certain breeds and managed case-by-case; related to uric acid)
- cystine (rare; genetic origin and often lifelong management; caused by an inherited amino acid handling problem)
Here are a few practical points to keep in mind:
- Male cats have a higher risk of a complete urethral blockage (urethral obstruction – a full stop that prevents urine from leaving the body).
- Do not try to pass a catheter at home – a catheter is a thin tube used to open the urethra and you can cause severe damage if you do it yourself.
- If you think your cat is blocked, follow the urgent-action block at the top of this article and go to the clinic right away.
- Bring any recent x-rays or ultrasound reports when you go to the clinic so the vet can compare images.
A urethral obstruction is a medical emergency. Your cat may strain, cry, pace, lick the area, or only produce tiny dribbles of urine. Untreated blockage can lead to kidney failure, a dangerous electrolyte imbalance (high potassium – called hyperkalemia), or even bladder rupture within 48 to 72 hours. Fast veterinary care can be lifesaving, so get your cat to the clinic as quickly as you can.
Feline idiopathic cystitis (FLUTD/FIC) and stress-related bladder bleeding

Feline idiopathic cystitis, or FIC (bladder inflammation with no clear cause), is a common noninfectious reason you might see blood in your cat’s urine. It falls under the bigger category called FLUTD (feline lower urinary tract disease), which just means problems in the bladder and urethra. Ever watched your cat squat and look uncomfortable? That’s the kind of thing we’re talking about.
Vets first rule out things we can treat, like infection (bacterial infection) and urinary stones (hard mineral crystals). They’ll check urine, do bloodwork, and sometimes run imaging (x-rays or ultrasound) to confirm hematuria (blood in urine) and find the cause , see How vets confirm hematuria for clinic tests and imaging details.
Practical prevention and home monitoring (owner-facing):
- Offer more wet food (canned food) to boost moisture intake.
- Add a cat water fountain (continuous-flow bowl) or other flowing water , many cats drink more from moving water.
- Put several fresh-water stations around the house and try shallow, wide dishes if your cat prefers them.
- Lower household stress with quiet resting spots, short regular play sessions, and easy-to-reach hiding places. Ever watched your kitty chase a ribbon and then flop down for a nap? That calm matters.
- Watch litter-box habits closely: note how often your cat urinates and what the urine looks like. Keep enough boxes , one per cat plus one extra , and place them in separate, quiet areas.
For the full prevention checklist and step-by-step home-care guidance, see the Treatment/Prevention section.
Worth every paw-print.
Causes of Blood in Cat Urine

Blunt trauma , from a fall, a cat fight, or being hit by a car , can nick the bladder (the small sac that holds urine), kidneys (the organs that filter blood), or urethra (the tube that carries urine out) and lead to visible blood in the urine. Sometimes there are no scratches or cuts on the fur to show something’s wrong, so if you know your cat was injured and you see blood, get them to the vet right away. They may need imaging like X-rays or an ultrasound, and sometimes surgical repair.
Example: He seemed fine after the scuffle, then his urine had blood , internal bladder tears can hide under unmarked fur. Ever see that? It’s scary.
Coagulopathy (a clotting disorder) can be something a cat is born with, a side effect of medications, or the result of toxins like anticoagulant rodenticide (rat poison that stops blood from clotting). You’ll often see bleeding from more than one spot: gums, skin bruises, nosebleeds, and bloody urine. Quick lab work such as clotting panels (blood tests that measure how fast blood clots) helps figure this out and guides treatment. Quick tip: if you suspect your cat ate bait or poison, tell the vet right away so they can run the right tests.
Less common causes include bladder cancer, which shows up more in cats over ten and usually causes ongoing blood in the urine plus unexplained weight loss, and systemic viruses like FeLV (feline leukemia virus) and FIV (feline immunodeficiency virus) that can raise bleeding risk. Advanced kidney infection, called pyelonephritis (kidney infection), can also cause bloody urine. It’s not always one thing, so vets look at the whole picture.
Red flags that mean you should get urgent veterinary care
- Any recent trauma or obvious injury. Imaging or surgery may be needed, and internal bruising can happen with no outside wounds.
- Bleeding from more than one place, like gums, skin, or the nose.
- Sudden extreme tiredness, easy bruising, or weakness.
- Known or suspected rodenticide exposure. Consider clotting panels (tests that check blood clotting).
- An older cat with persistent blood in the urine and weight loss.
What to expect at an emergency clinic

Start by following the urgent-action checklist at the top for immediate steps. When you get to the clinic, they’ll stabilize your cat first, then run the tests described in the diagnostics section. Note: owner cautions like "Do not attempt catheterization at home" and that male cats are at higher risk of complete urethral obstruction are placed in the urgent-action block so you can find them fast.
Ever watched your kitty suddenly stop peeing? That’s the kind of emergency this is, so staff move quickly.
- Stabilization and triage happen right away. They’ll check vital signs: temperature, heart rate, and breathing.
- Dangerous electrolyte imbalances get corrected with IV fluids (fluids given into a vein). They’ll also monitor for hyperkalemia (high potassium) using an ECG (electrocardiogram, a test that checks heart rhythm) and bloodwork.
- If the bladder is blocked, catheterization may be done under sedation. Catheterization (a thin tube placed to relieve a blockage) lets the bladder decompress and relieves the immediate danger. Please don’t try this at home.
- Your cat might be hospitalized for a while for monitoring, pain control, and urine-output checks (so the team can make sure your cat is actually peeing again).
Worth every paw-print.
Treatment options, recovery expectations, and a master prevention checklist

Follow the diagnosis-specific plan your vet gives you. See the UTI/pyelonephritis, stones, FLUTD, and How vets confirm hematuria sections for details. Meds and procedures are chosen based on tests, not guesses. For example: if a culture (a lab test that grows bacteria from urine) finds bacteria X, the vet will switch to drug Y for the best result.
Home support matters. Give medications exactly as directed. Boost hydration with canned food and a water fountain so your cat sips more (hydration helps flush the bladder). Watch the litter box and write down changes in color, amount, and how often your cat goes. Example note: "Day 3 , pale yellow, three small clumps, peed mid-day and evening."
Bring a fresh urine sample and clear photos to rechecks whenever you can. That really helps the clinic track color and volume changes. Photo tip: place a clean white paper under the litter area and zoom in on the wet spot to show color and size.
If your cat is straining, collapsing, or not producing urine, use the clinic’s emergency/obstruction guidance right away. Those signs can mean a urethral obstruction (a blocked urethra) and need urgent attention. The ER/obstruction section explains the next steps.
Follow the recheck schedule below for typical timing and what to bring, but always adjust to your vet’s plan.
| Condition | Typical recheck timing | What to bring |
|---|---|---|
| Uncomplicated lower UTI | Urinalysis (urine test) 7–14 days after finishing antibiotics | Fresh urine sample, list of meds, photo of any urine change |
| Pyelonephritis (kidney infection) | Culture (bacterial growth test) and/or urinalysis during therapy; repeat at 2–4 weeks and at end of the 4–6 week course | Fresh urine, prior culture results, any imaging reports |
| Stones (medical dissolution or post-op) | Imaging (x-ray or ultrasound) and urinalysis per surgeon/vet , commonly 2–6 weeks after treatment | Recent imaging (CD/USB/photos), urine sample, medication list |
| Post-urethral obstruction | Clinic recheck within 24–72 hours, then 7–14 days as advised | Fresh urine, photos, notes on litter-box behavior and meds |
Reminder: bring a fresh urine sample and photos to rechecks so the clinic can compare changes quickly. Worth every paw-print.
Final Words
In the action: fast triage steps, a clear shortlist of likely diagnoses, the full clinic test plan, and practical treatment plus prevention tips. You’ve got what to do right now and what vets will do next.
Keep calm, collect a safe sample or photo, and get help fast if your cat shows emergency signs. Small changes at home, more wet food, fresh water, quiet litter boxes, go a long way.
Stay hopeful. With quick action and steady care, you can protect playtime and spot the causes of blood in cat urine early.
FAQ
Causes of blood in cat urine (male)
The causes of blood in a male cat’s urine include urinary tract infection, feline lower urinary tract disease (FLUTD), bladder stones or urethral obstruction, trauma, clotting disorders, and less commonly bladder cancer.
Blood in cat urine (female)
The causes of blood in a female cat’s urine include urinary tract infection, FLUTD, bladder stones, reproductive tract bleeding, trauma, kidney infection, and clotting problems; UTIs are relatively more common in females.
Why is my cat peeing blood but acting normal?
If your cat is peeing blood but acting normal, the cause may be early UTI, FLUTD, small stones, or intermittent bleeding; cats often hide pain, so a vet exam and urinalysis are wise.
Blood in cat urine home remedies
Home remedies for blood in cat urine are limited; try offering canned food and fresh water, reduce stress, and keep litter-box records, but never give antibiotics or try home catheterization.
How do you treat blood in a cat’s urine?
Treatment depends on the cause: antibiotics guided by culture for bacterial infection, pain relief for cystitis, diet or surgery for stones, and fluids/catheterization for obstruction.
When is blood in cat urine an emergency?
Blood in cat urine is an emergency if your cat is straining with little or no urine, vomiting repeatedly, collapsing, breathing poorly, extremely lethargic, or has a tense, painful abdomen — get to a clinic now.